What device uses a light attached to look inside a body cavity or organ
| Endoscopy | |
|---|---|
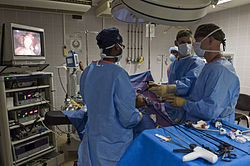
 An case of an endoscopic process | |
| MeSH | D004724 |
| OPS-301 code | 1-twoscore...1-49, ane-61...1-69 |
| MedlinePlus | 003338 |
An endoscopy (looking inside) is a process used in medicine to await inside the trunk.[1] The endoscopy procedure uses an endoscope to examine the interior of a hollow organ or cavity of the body. Unlike many other medical imaging techniques, endoscopes are inserted directly into the organ or orifices.
There are many types of endoscopies. Depending on the site in the body and type of procedure, an endoscopy is performed by an endoscopist who is typically either a md or a surgeon. A patient may be fully conscious or anaesthetised during the procedure. Most often, the term endoscopy is used to refer to an test of the upper part of the gastrointestinal tract, known as an esophagogastroduodenoscopy.[ii]
For nonmedical use, similar instruments are called borescopes.
History [edit]
Adolf Kussmaul was fascinated by sword swallowers who would insert a sword down their throat without gagging. This drew inspiration to insert a camera, the adjacent trouble to solve was how to insert a source of light, every bit they were still relying on candles and oil lamps.[iii]
The term endoscope was start used on February vii, 1855, past engineer-optician Charles Chevalier, in reference to the uréthroscope of Désormeaux, who himself began using the quondam term a month after.[four] The self-illuminated endoscope was developed at Glasgow Royal Infirmary in Scotland (i of the outset hospitals to have mains electricity) in 1894/5 past Dr John Macintyre as part of his specialization in investigation of the larynx.[5] [ failed verification ]
Medical uses [edit]

Performance part of the endoscope

Insertion tip of endoscope
Endoscopy may exist used to investigate symptoms in the digestive system including nausea, vomiting, intestinal pain, difficulty swallowing, and gastrointestinal bleeding.[6] It is also used in diagnosis, near commonly by performing a biopsy to cheque for conditions such as anemia, bleeding, inflammation, and cancers of the digestive system.[half-dozen] The procedure may also be used for treatment such as cauterization of a haemorrhage vessel, widening a narrow esophagus, clipping off a polyp or removing a foreign object.[6]
Specialty professional organizations that specialize in digestive problems advise that many patients with Barrett's esophagus receive endoscopies as well oftentimes.[7] Such societies recommend that patients with Barrett'due south esophagus and no cancer symptoms afterwards two biopsies receive biopsies equally indicated and no more ofttimes than the recommended rate.[eight] [9]
Applications [edit]

Health intendance providers can utilise endoscopy to review any of the following body parts:
- The gastrointestinal tract (GI tract):
- oesophagus, stomach and duodenum (esophagogastroduodenoscopy)

Esophageal Bougie Dilator
- minor intestine (enteroscopy)
- large intestine/colon (colonoscopy, sigmoidoscopy)
- Magnification endoscopy
- bile duct
- endoscopic retrograde cholangiopancreatography (ERCP), duodenoscope-assisted cholangiopancreatoscopy, intraoperative cholangioscopy
- rectum (rectoscopy) and anus (anoscopy), both also referred to as (proctoscopy)
-
- The respiratory tract
- The nose (rhinoscopy)
- The upper respiratory tract (laryngoscopy)
- The lower respiratory tract (bronchoscopy)
- The ear (otoscope)
- The urinary tract (cystoscopy)
- The female reproductive organisation (gynoscopy)
- The cervix (colposcopy)
- The uterus (hysteroscopy)
- The fallopian tubes (falloposcopy)
- Normally closed torso cavities (through a small incision):
- The abdominal or pelvic cavity (laparoscopy)
- The interior of a joint (arthroscopy)
- Organs of the chest (thoracoscopy and mediastinoscopy)
Endoscopy is used for many procedures:
- During pregnancy
- The amnion (amnioscopy)
- The fetus (fetoscopy)
- Plastic surgery
- Panendoscopy (or triple endoscopy)
- Combines laryngoscopy, esophagoscopy, and bronchoscopy
- Orthopedic surgery
- Paw surgery, such as endoscopic carpal tunnel release
- Human knee surgery, such equally anterior cruciate ligament reconstruction
- Epidural space (Epiduroscopy)
- Bursae (Bursectomy)
- Endodontic surgery
- Maxillary sinus surgery
- Apicoectomy
- Endoscopic endonasal surgery
- Endoscopic spinal surgery
An Endoscopy is a elementary process that allows a doctor to expect inside human bodies using an musical instrument called an endoscope. A cutting tool can exist fastened to the end of the endoscope, and the appliance tin can then exist used to perform modest procedures such as tissue biopsies, banding of oesophageal varices or removal of polyps.
Application in other fields [edit]
- For non-medical use, such every bit internal inspection of complex technical systems, borescopes are used. These are like to endoscopes.
- The planning and architectural community utilise architectural endoscopy for pre-visualization of scale models of proposed buildings and cities
- Endoscopes are also a tool helpful in the exam of improvised explosive devices by bomb disposal personnel.
- Law enforcement uses endoscopes for conducting surveillance via tight spaces.
Risks [edit]
The main risks are infection, over-sedation, perforation, or a tear of the stomach or esophagus lining and bleeding.[10] Although perforation generally requires surgery, sure cases may exist treated with antibiotics and intravenous fluids. Bleeding may occur at the site of a biopsy or polyp removal. Such typically minor bleeding may only stop on its ain or exist controlled by cauterisation. Seldom does surgery get necessary. Perforation and bleeding are rare during gastroscopy. Other minor risks include drug reactions and complications related to other diseases the patient may take. Consequently, patients should inform their medico of all allergic tendencies and medical problems. Occasionally, the site of the allaying injection may become inflamed and tender for a short time. This is usually not serious and warm compresses for a few days are commonly helpful. While any of these complications may possibly occur, each of them occurs quite infrequently. A doctor can farther hash out risks with the patient with regard to the particular need for gastroscopy.
Later the endoscopy [edit]
Later on the procedure, the patient volition exist observed and monitored past a qualified individual in the endoscopy room, or a recovery area, until a significant portion of the medication has worn off. Occasionally the patient is left with a mild sore pharynx, which may respond to saline gargles, or chamomile tea. Information technology may last for weeks or not happen at all. The patient may have a feeling of distention from the insufflated air that was used during the procedure. Both problems are mild and fleeting. When fully recovered, the patient will exist instructed when to resume their usual diet (probably within a few hours) and volition exist allowed to be taken domicile. Where sedation has been used, most facilities mandate that the patient be taken home by another person and that they not bulldoze or handle machinery for the rest of the 24-hour interval. Patients who take had an endoscopy without sedation are able to leave unassisted.
Endoscope [edit]
An endoscope tin consist of:
- a rigid or flexible tube.
- a light delivery system to illuminate the organ or object nether inspection. The light source is normally outside the body and the low-cal is typically directed via an optical cobweb system.
- a lens system transmitting the image from the objective lens to the viewer, typically a relay lens system in the case of rigid endoscopes or a bundle of fiberoptics in the case of a fiberscope.
- an eyepiece. Modern instruments may be videoscopes, with no eyepiece. A photographic camera transmits epitome to a screen for epitome capture.
- an additional channel to allow entry of medical instruments or manipulators.
Patients undergoing the procedure may be offered sedation, which includes its own risks.
History [edit]

Drawings of Bozzini's "Lichtleiter", an early on endoscope
The first endoscope was developed in 1806 by Philipp Bozzini in Mainz with his introduction of a "Lichtleiter" (light conductor) "for the examinations of the canals and cavities of the human body".[11] However, the College of Physicians in Vienna disapproved of such marvel.[12] The first to apply an endoscope in a successful operation was Antonin Jean Desormeaux whose invention was the state of the art earlier the invention of electricity.[4]
The apply of electrical light was a major step in the improvement of endoscopy. The start such lights were external although sufficiently capable of illumination to allow cystoscopy, hysteroscopy and sigmoidoscopy besides as examination of the nasal (and later thoracic) cavities as was being performed routinely in man patients past Sir Francis Cruise (using his own commercially available endoscope) by 1865 in the Mater Misericordiae Hospital in Dublin, Ireland.[13] Later, smaller bulbs became bachelor making internal low-cal possible, for instance in a hysteroscope past Charles David in 1908.[fourteen]
Hans Christian Jacobaeus has been given credit for the first large published series of endoscopic explorations of the abdomen and the thorax with laparoscopy (1912) and thoracoscopy (1910)[15] although the kickoff reported thoracoscopic examination in a man was also by Cruise.[16]
Laparoscopy was used in the diagnosis of liver and gallbladder disease by Heinz Kalk in the 1930s.[17] Hope reported in 1937 on the apply of laparoscopy to diagnose ectopic pregnancy.[18] In 1944, Raoul Palmer placed his patients in the Trendelenburg position after gaseous distention of the abdomen and thus was able to reliably perform gynecologic laparoscopy.[19]
Wolf and Storz [edit]
Georg Wolf (1873–1938) a Berlin manufacturer of rigid endoscopes, established in 1906, produced the Sussmann flexible gastroscope in 1911 (Modlin, Farhadi-Journal of Clinical Gastroenterology, 2000).[twenty] Karl Storz began producing instruments for ENT specialists in 1945 through his company, Karl Storz GmbH.[21]
Fiber optics [edit]

Basil Hirschowitz and Larry Curtiss invented the first cobweb optic endoscope in 1957.[22] Earlier in the 1950s Harold Hopkins had designed a "fibroscope" consisting of a bundle of flexible glass fibres able to coherently transmit an image. This proved useful both medically and industrially, and subsequent inquiry led to further improvements in image quality. Further innovations included using boosted fibres to channel light to the objective end from a powerful external source, thereby achieving the high level of total spectrum illumination that was needed for detailed viewing, and colour photography.[ commendation needed ]
The previous practice of a small filament lamp on the tip of the endoscope had left the selection of either viewing in a dim cherry light or increasing the light output - which carried the hazard of burning the inside of the patient. Alongside the advances to the optics, the ability to 'steer' the tip was developed, too as innovations in remotely operated surgical instruments contained inside the torso of the endoscope itself. This was the beginning of "key-hole surgery" as nosotros know information technology today.[23]
Rod-lens endoscopes [edit]
At that place were physical limits to the image quality of a fibroscope. A bundle of say 50,000 fibers gives effectively only a 50,000-pixel image, and continued flexing from use breaks fibers and and so progressively loses pixels. Eventually so many are lost that the whole bundle must be replaced (at considerable expense). Harold Hopkins realised that any further optical improvement would crave a different approach. Previous rigid endoscopes suffered from low light transmittance and poor image quality. The surgical requirement of passing surgical tools as well equally the illumination system inside the endoscope's tube - which itself is limited in dimensions by the homo trunk - left very lilliputian room for the imaging optics. The tiny lenses of a conventional system required supporting rings that would obscure the majority of the lens area; they were difficult to manufacture and assemble and optically virtually useless.[ citation needed ]
The elegant solution that Hopkins invented was to make full the air-spaces between the 'little lenses' with rods of glass. These fitted exactly the endoscope'southward tube, making them self-aligning, and required no other support. This allowed the lilliputian lenses to exist dispensed with altogether. The rod-lenses were much easier to handle and used the maximum possible diameter bachelor.[ commendation needed ]
With the appropriate curvature and coatings to the rod ends and optimal choices of glass-types, all calculated and specified by Hopkins, the epitome quality was transformed - even with tubes of but 1mm in bore. With a high quality 'telescope' of such small bore the tools and illumination system could be comfortably housed within an outer tube. Once again it was Karl Storz who produced the beginning of these new endoscopes equally part of a long and productive partnership betwixt the two men.[24]
Whilst at that place are regions of the body that will always require flexible endoscopes (principally the alimentary canal), the rigid rod-lens endoscopes take such exceptional performance that they are still the preferred instrument and take enabled modern cardinal-hole surgery. (Harold Hopkins was recognized and honoured for his advancement of medical-optic by the medical community worldwide. It formed a major part of the commendation when he was awarded the Rumford Medal by the Purple Society in 1984.)
Past measuring assimilation of light by the blood (by passing the light through one fibre and collecting the light through another fibre) a dr. can estimate the proportion of haemoglobin in the blood and diagnose ulceration in the breadbasket.[ commendation needed ]
Endoscope reprocessing [edit]
High level disinfection of flexible endoscopes is required by all national guideline issuing bodies.[25] The high level disinfection of endoscopes occurs during a multi-stride process called reprocessing. Reprocessing endoscopes involves over 100 individuals steps.[26] These steps can exist broken down into broad categories of pre-cleaning, leak testing, transmission cleaning, cleaning verification, visual inspection, high level disinfection, rinsing, drying, and storage.[27] Failure to perform all of these steps correctly can atomic number 82 to residual contagion remaining on endoscopes.
In the UK, stringent guidelines exist regarding the decontamination and disinfection of flexible endoscopes, the most contempo existence CfPP 01–06, released in 2013[28]
Rigid endoscopes, such as an Arthroscope, tin be sterilized in the aforementioned way as surgical instruments, whereas heat labile flexible endoscopes cannot.[29]
Recent developments [edit]

Low-cost waterproof USB endoscope for non-medical use.
With the application of robotic systems, telesurgery was introduced equally the surgeon could be at a site far removed from the patient. The commencement transatlantic surgery has been called the Lindbergh Functioning.[ commendation needed ]
Wireless oesophageal pH measuring devices can now be placed endoscopically, to tape ph trends in an area remotely.[ commendation needed ]
Endoscopy VR simulators [edit]
Virtual reality simulators are beingness developed for training doctors on diverse endoscopy skills.[xxx]
Dispensable endoscopy [edit]
Disposable endoscopy is an emerging category of endoscopic instruments. Recent developments[31] have allowed the industry of endoscopes inexpensive enough to be used on a single patient only. It is meeting a growing need to lessen the risk of cantankerous contamination and hospital acquired diseases. A European consortium of the SME is working on the DUET (disposable employ of endoscopy tool) project to build a disposable endoscope.[32]
Video Capsule endoscopy [edit]
Sheathing endoscopes are pill-sized imaging devices that are swallowed by a patient so record images of the gastrointestinal tract equally they laissez passer through naturally. Images are typically transmitted wirelessly to an external receiver. Capsule endoscopes may be expensive because they are excreted and are usable merely one time.
Augmented reality [edit]
The endoscopic image tin be combined with other paradigm sources to provide the surgeon with additional information. For instance, the position of an anatomical construction or tumor might exist shown in the endoscopic video.[33]
New imaging modalities [edit]
Emerging endoscope technologies measure additional properties of calorie-free to improve contrast, such equally optical polarization,[34] optical phase,[35] and additional wavelengths of light (hyperspectral endoscopy).[36]
See besides [edit]
- Colonoscopy
- Enteroscopy
- Surgery
- Anesthesia
References [edit]
- ^ "Endoscopy". British Medical Association Complete Family Health Encyclopedia. Dorling Kindersley Limited. 1990.
- ^ "Endoscopy". Cancer Research Great britain. Retrieved 5 November 2015.
- ^ "The pioneers of endoscopy and the sword swallowers".
- ^ a b Janssen, Diederik F (2021-05-17). "Who named and built the Désormeaux endoscope? The case of unacknowledged opticians Charles and Arthur Chevalier". Journal of Medical Biography. 29 (3): 176–179. doi:10.1177/09677720211018975. ISSN 0967-7720. PMID 33998906. S2CID 234747817.
- ^ "The Scottish Society of the History of Medicine" (PDF).
- ^ a b c Staff (2012). "Upper endoscopy". Mayo Clinic . Retrieved 24 September 2012.
- ^ American Gastroenterological Association, "Five Things Physicians and Patients Should Question" (PDF), Choosing Wisely: an initiative of the ABIM Foundation, American Gastroenterological Association, archived from the original (PDF) on August ix, 2012, retrieved August 17, 2012
- ^ Spechler SJ, Sharma P, Souza RF, Inadomi JM, Shaheen NJ (March 2011). "American Gastroenterological Association medical position statement on the management of Barrett's esophagus". Gastroenterology. 140 (three): 1084–91. doi:ten.1053/j.gastro.2011.01.030. PMID 21376940.
- ^ Wang KK, Sampliner RE (March 2008). "Updated guidelines 2008 for the diagnosis, surveillance and therapy of Barrett's esophagus". The American Journal of Gastroenterology. 103 (3): 788–97. doi:10.1111/j.1572-0241.2008.01835.10. PMID 18341497. S2CID 8443847.
- ^ "Endoscopy". NHS Choices. NHS Gov.United kingdom of great britain and northern ireland. Retrieved April 20, 2017.
- ^ Bozzini, Philipp (1806). "Lichtleiter, eine Erfindung zur Anschauung innerer Teile und Krankheiten, nebst der Abbildung" [Light conductor, an invention for examining internal parts and diseases, together with illustrations]. Periodical der Practischen Arzneykunde und Wundarzneykunst (in German). 24: 107–24.
- ^ Yamada T (2009-01-22). Atlas of Gastroenterology. John Wiley & Sons. ISBN978-1-4443-0342-1.
- ^ Caniggia A, Nuti R, Lore F, Martini G, Turchetti V, Righi G (April 1990). "Long-term treatment with calcitriol in postmenopausal osteoporosis". Metabolism. 39 (4 Suppl one): 43–9. doi:10.1136/bmj.1.223.345. JSTOR 25204557. PMC2325571. PMID 2325571.
- ^ Shawki O, Deshmukh S, Pacheco LA (2017). Mastering the Techniques in Hysteroscopy. Jaypee Brothers Medical Publishers. pp. 13–. ISBN978-93-86150-49-3.
- ^ Litynski GS (January–Mar 1997). "Laparoscopy--the early attempts: spotlighting Georg Kelling and Hans Christian Jacobaeus". JSLS. 1 (one): 83–five. PMC3015224. PMID 9876654.
- ^ Gordon S (2014). "Fine art. 8.—Clinical reports of rare cases, occurring in the Whitworth and Hardwicke Hospitals". Dublin Quarterly Journal of Medical Science. 41 (1): 83–99. doi:x.1007/BF02946459.
- ^ Wildhirt Eastward, Kalk H (1977). Neue Deutsche Biographie (NDB). Ring 11. Berlin: Duncker & Humblot. p. 60. ISBN978-3-428-00192-7.
- ^ Balen AH, Creighton SM, Davies MC, MacDougall J, Stanhope R (2004-04-01). Paediatric and Adolescent Gynaecology: A Multidisciplinary Approach. Cambridge University Printing. pp. 131–. ISBN978-1-107-32018-5.
- ^ Litynski GS (Jul–Sep 1997). "Raoul Palmer, Globe War Ii, and transabdominal coelioscopy. Laparoscopy extends into gynecology". Journal of the Society of Laparoendoscopic Surgeons. one (3): 289–92. PMC3016739. PMID 9876691.
- ^ "Near Richard Wolf Federal republic of germany". Richard Wolf Medical Instruments.
- ^ Nezhat C (2005). "Chapter xix. 1960's". Nezhat's History of Endoscopy. Society of Laparoendoscopic Surgeons. Archived from the original on 2018-07-27. Retrieved 2016-01-07 .
- ^ Edmonson JM (March 1991). "History of the instruments for gastrointestinal endoscopy". Gastrointestinal Endoscopy. 37 (2 Suppl): S27–56. doi:x.1016/S0016-5107(91)70910-three. PMID 2044933.
- ^ Sun, Guoging; et al. (January 2019). "Comparison of keyhole endoscopy and craniotomy for the treatment of patients with hypertensive cerebral hemorrhage". Medicine. Baltimore. 98 (2): e14123. doi:x.1097/Doctor.0000000000014123. PMC6336657. PMID 30633227.
- ^ "History". Harold Hopkins Society.
- ^ Ofstead CL, Wetzler HP, Heymann OL, Johnson EA, Eiland JE, Shaw MJ (February 2017). "Longitudinal assessment of reprocessing effectiveness for colonoscopes and gastroscopes: Results of visual inspections, biochemical markers, and microbial cultures". American Journal of Infection Control. 45 (2): e26–e33. doi:10.1016/j.ajic.2016.10.017. PMID 28159069. S2CID 19079905.
- ^ Ofstead CL, Wetzler HP, Snyder AK, Horton RA (2010). "Endoscope reprocessing methods: a prospective written report on the impact of man factors and automation". Gastroenterology Nursing. 33 (4): 304–11. doi:ten.1097/SGA.0b013e3181e9431a. PMID 20679783. S2CID 206060013.
- ^ Herrin A, Loyola M, Bocian S, Diskey A, Friis CM, Herron-Rice L, Juan MR, Schmelzer M, Selking S (2016). "Standards of Infection Prevention in Reprocessing Flexible Gastrointestinal Endoscopes". Gastroenterology Nursing. 39 (5): 404–eighteen. doi:x.1097/SGA.0000000000000266. PMID 27684640. S2CID 37069977.
- ^ "Wellness Technical Memorandum 01-06: Decontamination of exible endoscopes Part C: Operational management" (PDF). Great britain Department of Wellness. March 2016.
- ^ Sabnis RB, Bhattu A, Vijaykumar 1000 (March 2014). "Sterilization of endoscopic instruments". Current Stance in Urology. 24 (ii): 195–202. doi:x.1097/MOU.0000000000000034. PMID 24451088. S2CID 29328096.
- ^ "Overview of Endoscopy Haptics Simulator Projection". M2D2 Laboratory, Indian Plant of Science. YouTube.
- ^ "Dokument nicht gefunden". Archived from the original on 2011-07-twenty.
- ^ "Development of a Dispensable Apply Endoscopy Tool". 2018-03-26. Archived from the original on 2011-07-23.
- ^ Augmented Reality: Path guidance to craniopharyngioma on YouTube
- ^ Manhas S, Vizet J, Deby S, Vanel JC, Boito P, Verdier M, De Martino A, Pagnoux D (February 2015). "Demonstration of full 4×iv Mueller polarimetry through an optical fiber for endoscopic applications". Optics Express. 23 (iii): 3047–54. Bibcode:2015OExpr..23.3047M. doi:10.1364/OE.23.003047. PMID 25836165.
- ^ Gordon, GSD; Joseph, J; Alcolea, MP; Sawyer, T; Macfaden, AJ; Williams, C; Fitzpatrick, CRM; Jones, PH; di Pietro, M; Fitzgerald, RC; Wilkinson, TD; Bohndiek, SE (2018). "Quantitative stage and polarisation endoscopy applied to detection of early oesophageal tumourigenesis". Journal of Biomedical Optics. 24 (12): 1–13. arXiv:1811.03977. doi:x.1117/1.JBO.24.12.126004. PMC7006047. PMID 31840442.
- ^ Kester RT, Bedard N, Gao L, Tkaczyk TS (May 2011). "Real-time snapshot hyperspectral imaging endoscope". Journal of Biomedical Eyes. xvi (v): 056005–056005–12. Bibcode:2011JBO....16e6005K. doi:10.1117/1.3574756. PMC3107836. PMID 21639573.
External links [edit]
| | Wikimedia Eatables has media related to Endoscopy. |
- The Atlas of Gastrointestinal Endoscopy endoatlas.com
- El Salvador Atlas of Gastrointestinal Endoscopy
- Gastrolab: Site in English, Swedish and Finnish with gastrointestinal endoscopy photolibrary Archived 2020-07-x at the Wayback Machine
- Preventing cross-contagion from flexible endoscopes massdevice.com
- Advances in Endoscopy Archived 2018-05-thirteen at the Wayback Machine advancedimagingpro.com
Source: https://en.wikipedia.org/wiki/Endoscopy
0 Response to "What device uses a light attached to look inside a body cavity or organ"
Post a Comment